Patient Stories
For more parent resources and family experiences of neonatal care head over to: https://www.neonatalnetwork.co.uk
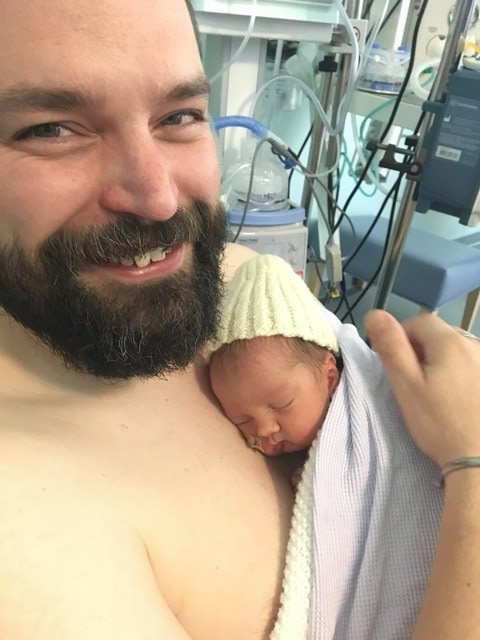
A Fathers Experience of a Neonatal Unit
Our third daughter was not supposed to be born 140 miles away. We were on a family holiday in the Forest of Dean, celebrating my mums 70th birthday. My partner was 34 weeks pregnant, and this was to be the last trip before hospital bags were going to be packed and birthing plans written etc.
As a father of two children already, I was pretty confident I had seen it all. Our eldest daughter was breech and born via what was supposed to be a planned caesarean, only she tried to arrive a day early, with a resulting ambulance trip into hospital. During her pregnancy with our second daughter my partner contracted chicken pox, which resulted in lots of stress and extra scans, but ultimately ended in the natural delivery of a healthy baby.
So, when my partner announced at the entrance to a local tourist attraction that the general discomfort she had been feeling was arranging itself into what appeared to be contractions, I was reasonably calm. A chat with our midwife via phone suggested a precautionary trip to the local hospital for a “routine check”. Still reasonably calm whilst googling local maternity units, I was mainly feeling a little grumpy that I was missing a good day out.
The NHS is amazing. We presented ourselves at the admission window of the maternity unit at the nearest hospital and in no time at all were booked into the observation suite and being taken care of. Drugs were administered to delay the onset of birth and one of those monitors involving blue and pink elastic bands was strapped on (and then moved, jiggled, poked, repositioned, taken off, put back on and jiggled some more).
I had complete faith in the ability of the drugs administered to stop the progression of labour, even when the first set failed to do anything. I thought we were going home later, with a little story to tell. My partner, however, says that at this point she knew that we weren’t leaving until the baby was born.
Even at the point the second stronger drip administered medication wasn’t doing much and they moved us into the delivery suite “just in case” I was still sure we were about to go home. However, labour then progressed very, very quickly and it became apparent, even to me, that baby was coming out.
NICU staff arrived, discussing what might happen next – at 34-weeks gestation she may or may not need some level of support with temperature, breathing and feeding. They readied the baby crash cart in the corner, which was odd, as for the previous two births I had examined these with a morbid curiosity and filed them away as things that happened to other people’s babies.
Baby daughter number 3 (Maija) was born at 23:42 and weighed 2.58kg. Initially fine, she quickly started to struggle with breathing. She was packed up onto a transport cot and wheeled off, with me in hot pursuit, having abandoned my partner in the delivery suite.
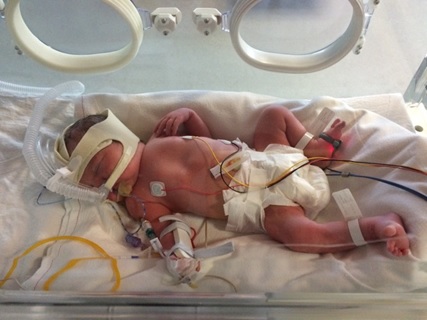
Going into the NICU for the first time was a shock – on some level I knew that intensive care units for babies existed, but I’d never given it any more thought than that and certainly hadn’t expected to find myself watching the careful installation of feeding tubes and cannulas and the hooking up of monitors to my daughter, who looked very small, naked in her heated incubator. At some point later that night my partner caught up with us having ‘recovered’ from the birth – she is luckily much tougher than me!
The next 24 hours for me was a series of logistical challenges involving existing children, holiday cottages, grandparents, work and late-night dashes back home to sort out more clothes and a hungry cat, whilst my partner established a pumping regime and kept watch over Maija. The staff were exceptionally helpful arranging temporary accommodation for us and putting up with our near constant presence on the ward – as visitors to the area, we had nowhere else to go.
We spent 2 weeks away from home, going through what at the time felt like never ending challenges, but with the benefit of some time and distance I realise were a pretty standard series of yellow alarms, red alarms, apnoeic episodes, worrying, tube feeding, sterilising, nappy changing though portholes, sterilising, awkward skin to skin cuddles involving wires tubes and worrying. Sterilising. Lots of worrying. Some more sterilising. Very little sleeping. Throughout though, the staff were amazing – I had faith in all of them, everything was explained and all the babies received excellent care and attention.
At the end of this period Maija was deemed fit to travel, and a cot had become free at our local unit in the North West, so it was time for a transfer. Mid-afternoon two enormous paramedics and two nurses appeared with a transport cot, and proceeded to ‘pack’ Maija using soft velcro strapping and wedges of foam into the capsule. Then they were all gone, off in an ambulance with the lights on, leaving us to trail behind in the car with a family sized cool box full of frozen breast milk in tiny bottles….
The adventure continued at our local unit. The nursing team helped us get breast feeding established, showed us how to safely bath a smaller than average baby (they really are slippery when wet) and made sure we were confident in giving her medication and basic first aid. All this was much more than I’d ever been shown prior to leaving hospital with my other daughters, which really helped my confidence when the time came for us to be discharged home.
At the time I first wrote this she had reached 9 months old. She was still smaller than her sisters were at the same age, and was often dwarfed by babies of a similar age. She was a bit behind with her milestones, but an exceptionally happy baby who was heading in the right direction.
She is now 2 and a half and still a very calm and happy toddler who is very chatty. She’s still on the smaller side, and a bit wobbly on her feet, but she’s catching up fast with her sisters.